Episode #37: Justin Lautenbach, From Orthopaedic Surgery to Aesthetic Injector
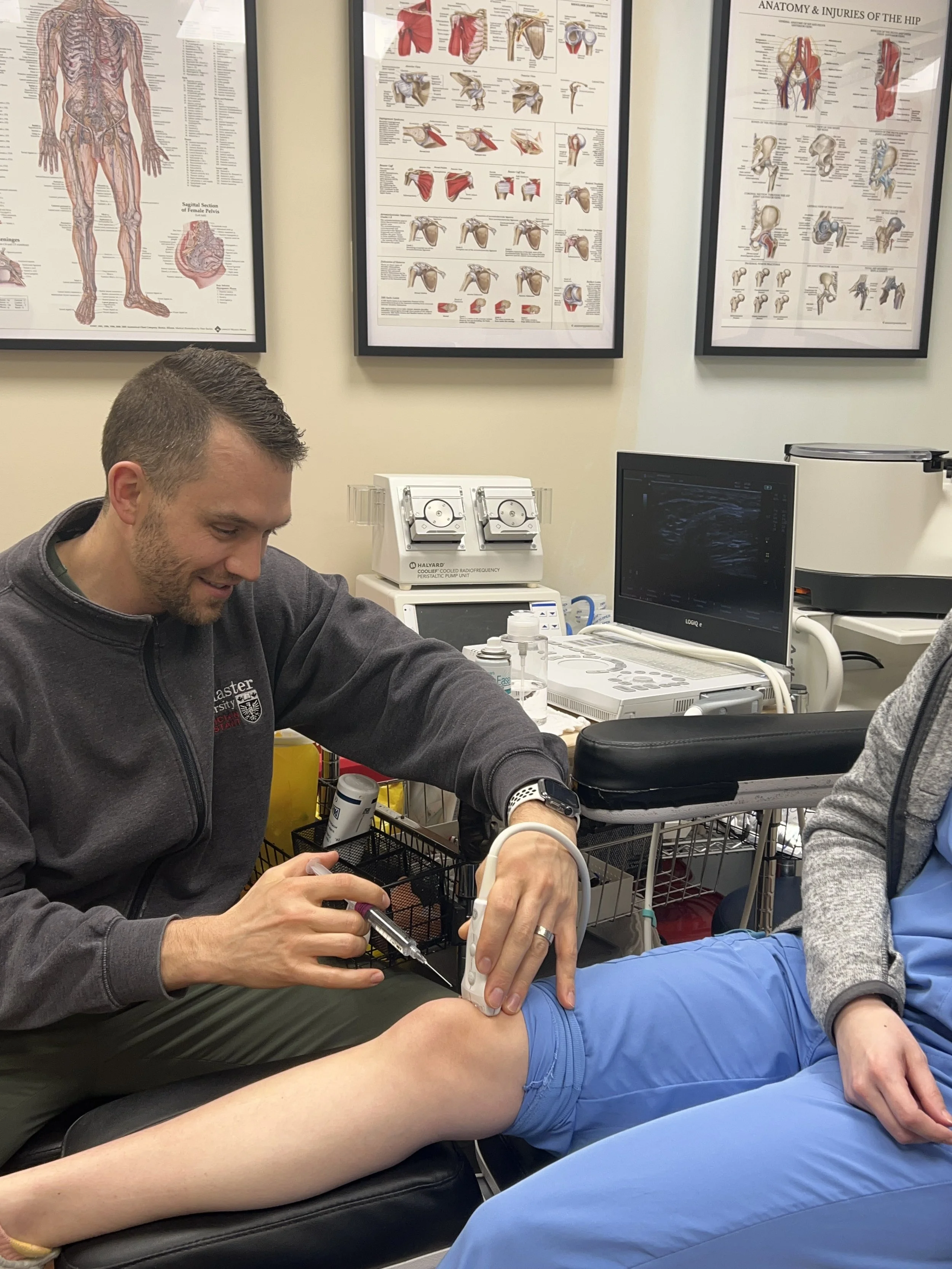
Justin performing an ultrasound guided knee injection.
Justin Lautenbach is a McMaster-trained PA who has spent over a decade building a multi-specialty career that spans outpatient Orthopedics, chronic pain, and now aesthetic medicine under his own brand, Hamilton Botox.
WHAT YOU’LL LEARNHow to move from a PA student in clinical clerkship to a licensed, practicing PA in Orthopaedic Surgery
What milestones are required to co-found and manage an outpatient medical practice
How to master ultrasound guided injections, procedures through pattern recognition and expert feedback
What the physician-directed model looks like for PAs in the business of aesthetic medicine
GUEST BIOJustin is a Canadian Physician Assistant with over a decade of experience in orthopaedic surgery, chronic pain management, and ultrasound-guided interventional care. He earned his undergraduate degree in Health Science from Brock University before entering the Physician Assistant Education Program at McMaster University in 2011, graduating in 2013.
He began his career at Brantford General Hospital working alongside Dr. Rabinovich in Orthopaedic Surgery. In 2016, Justin helped transition out of the hospital setting to co-found ArthroBiologix, an outpatient orthopaedic practice specializing in ultrasound-guided injection therapy and regenerative-focused care. During this time, he also began working in chronic pain management at Burlington Pain Care with Dr. Michael Boucher, where he continues to practice one day per week. In parallel, Justin gained experience in the medical insurance sector, completing intake assessments for independent medical examinations.
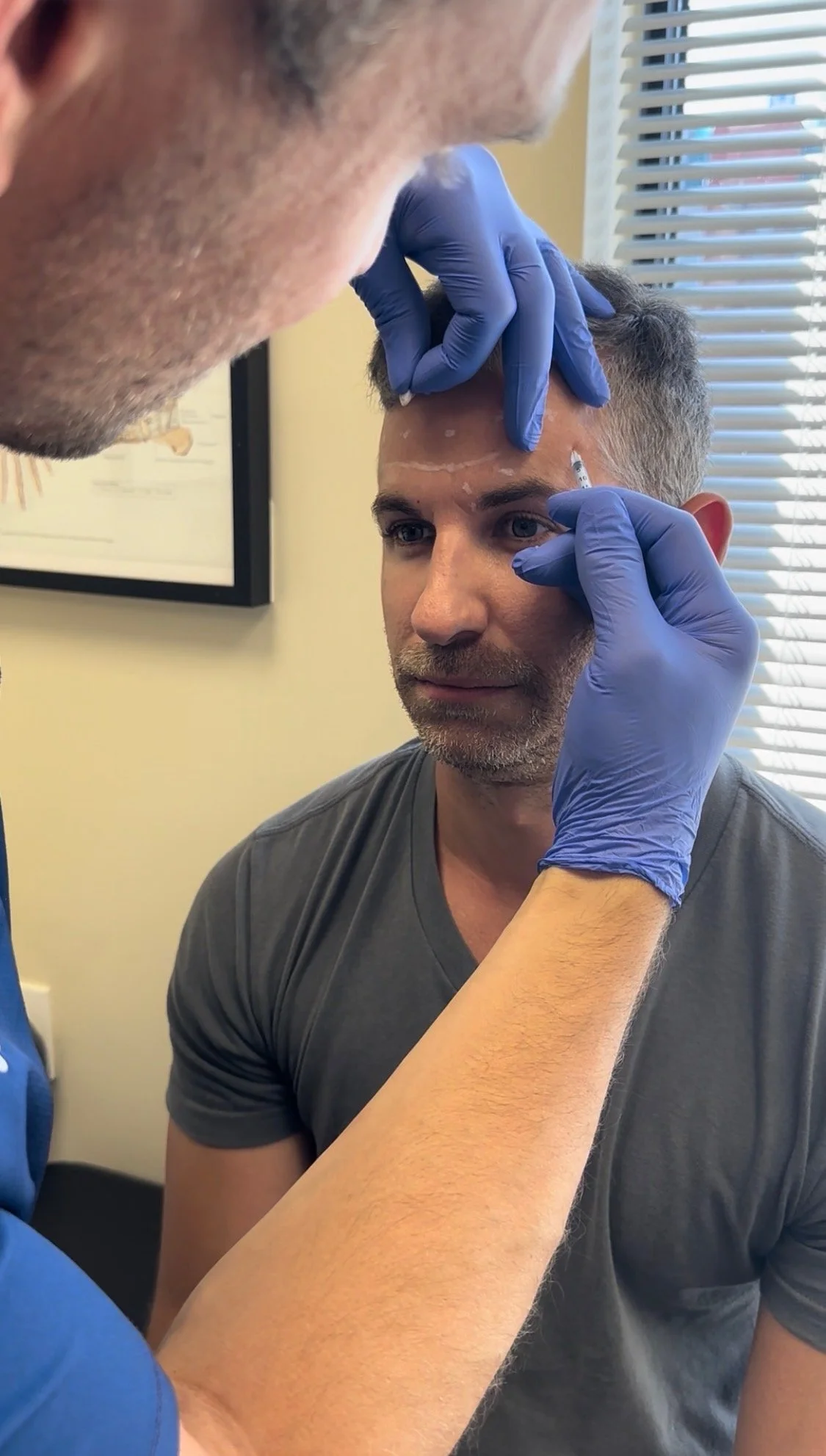
Through his chronic pain work, Justin treats a high volume of patients with migraines, where Botox has proven to be an effective and evidence-based therapy. As his experience grew, many patients also appreciated the secondary cosmetic benefits of treatment, which sparked a deeper interest in aesthetic medicine. In September 2024, Justin completed formal cosmetic Botox training with Dr. Rouzati through the National Academy of Aesthetic Medicine.
In September 2025, Justin founded Hamilton Botox, a practice that reflects his entrepreneurial approach to healthcare, combining medical expertise, procedural precision, and patient-centered care within a physician-directed model. He works under a medical directive with Dr. Abuelalaa and continues to balance clinical practice with business ownership, offering a unique perspective on the evolving role of Physician Assistants as both clinicians and healthcare entrepreneurs.
ON CAREER REINVENTION AS A PA“I went from Orthopaedics, to Pain Care, to now running my own Aesthetics company (@HamiltonBotox).
The PA profession gave me the flexibility to do all of that. Nobody handed it to me. I just kept saying ‘yes’ to what excited me.”
— Justin Lautenbach, CCPA
ON THE LEARNING CURVE IN YOUR FIRST PA JOB“I graduated, I was so excited to start contributing and then I quickly realized how incompetent I was. I had all the knowledge, but I wasn't applicable. That feeling of inadequacy humbled me, and I needed it.
You're not expected to graduate and all of a sudden be this amazing contributor right off the bat. Those first three to six months, stick with it. The skills come. It's just not an immediate process.”
— Justin Lautenbach, CCPA
ON BURNOUT EVEN IN A SPECIALTY YOU LOVE“If it doesn't feel right, it's probably not right. You can love your work and still burn out if you don't like who you're working with every day. That relationship goes both ways.”
— Justin Lautenbach, CCPA
ON PATIENT COMMUNICATION“How we explain something to patients really shapes how they experience it. It's less about saying the right thing— it's about learning to say things in the right way.”
— Justin Lautenbach, CCPA
ON PIONEERING THE PA PROFESSION, 10+ YEARS IN“The ceiling for what a PA can do in this country hasn't been hit yet. We're still figuring it out. And that's not a weakness — that's an opportunity.”
— Justin Lautenbach, CCPA
-
Introduction: Meet Justin
Justin[0:40] I came from an undergraduate degree in health science at Brock University. I graduated from there in 2011, and then I started the McMaster PA Education Program that same year and graduated in 2013. I started my initial position in Orthopaedics with Dr. Rabinovich at the Bradford General Hospital in November 2013. Then in 2016, we left the hospital and started an outpatient Orthopaedic practice that has since evolved into ArthroBiologix, which I think we'll touch on a little bit. At that same time, just due to the nature of the change, I started working in pain care in Burlington at a clinic called Burlington Pain Care with a couple of great physicians there as well. The nature of the evolution of ArthroBiologix has gotten really busy — I've stepped back a bit from Burlington Pain Care, but I'm there one day a week and I'm working at ArthroBiologix four days a week. So I'm pretty much Monday to Friday now, split 80/20 between the two clinics.
Anne[1:37] So you technically work in three specialties at once.
Justin[1:40] I'm working in outpatient Orthopaedics and chronic pain, and now in the last two years, I've been starting this aesthetic Botox company on my own, which is taking up a lot more time on top of the other two positions. That's been something I've been really passionate about in the last year especially, but really the last two years. So ArthroBiologix is an outpatient Orthopaedic practice, then there's the chronic pain, and now a little bit of aesthetic medicine on the side.
Anne[2:10] Fantastic. I'd like to take things back a few years. What drew you to the profession and how did your path unfold before getting into McMaster's PA program?
Justin[2:19] Much like yourself, I was one of the earlier classes, graduating in 2013. When I was going to Brock University, I was part of a program called Med Plus. It's an extracurricular program for people that are interested in medicine — it could be any profession — and we got introduced to physiotherapists, occupational therapists, chiros, and different medical specialties. I wasn't sure exactly what I wanted to do. I was pursuing medicine but wasn't really headstrong on the long haul of applying and going through all of that. In my third year, I had one of the first graduating classes come in — Donna — she works in family medicine in Niagara, and she came and told us about the PA profession. I'd never even heard of a PA. She was sitting there telling us about this profession, her quality of life, what she could do, the training. I left that day and I was like, I'm going to become a Physician Assistant. It ticked every box for me — being patient-facing without the long haul of medicine, but I could still practice in fields I was excited about. I had that 30-minute session with Donna and I knew that's what I wanted to do.
Justin's First Job as an Orthopaedic Surgery PA
Anne[3:26] You went to McMaster's PA program — two years, first year didactic, second is clerkship. Looking back from where you're sitting now, what did PA school actually prepare you for and what did it leave you to figure out on your own?
Justin[3:39] Like all of us, the two years is a whirlwind. It's such a blur and you're learning so much — but it's just continuous. You learn one thing and then in the next class you're learning something different, and then you try to apply that knowledge in your second year of clerkship. But I think beyond the science, beyond the medical education, the biggest takeaway was the need for communication and how communication is a clinical skill all on its own. How we explain something to patients really shapes how they experience it. When a patient feels confused, they're a little more anxious. When a patient's a little more anxious, they experience pain differently and outcomes tend to suffer a bit. Being able to reframe medical knowledge for patients in a way they can understand is so important — it allows you to build trust. And when patients trust you, outcomes get better. They're more likely to follow your medical plan. So for me, it was less about the medical knowledge itself and more about how good some practitioners are with communication and how much farther it goes. Learning to say things in the right way rather than just the right thing.
Anne[4:51] Your first role was in Orthopaedic surgery. What did that job teach you, apart from the communication piece?
Justin[5:02] I graduated and I started work and I was so excited to start contributing and being a Physician Assistant and getting paid — you're excited to start doing the job. Then I quickly realized how incompetent I was. I had all this knowledge and these skills, but I wasn't that applicable. Starting as a new grad felt very much like starting a new placement, except the expectations are higher. You're getting paid. You feel like you should be contributing more, but you still feel like a learner. For new PAs especially, I think it's good to just take a step back and realize the journey — the learning doesn't end, especially in those first six months to two years. There's so much learning. I just remember that feeling of inadequacy, how humbled I felt, and knowing I had a long ways to go. It's a long road to get to having expert skills at anything. You have to stick with it and continue to learn. Put in the hours and those skill sets start to come and you build on them and start to feel more competent. But it's not an immediate process. Those first three to six months can be daunting. The key is just sticking with it and appreciating that that's the expectation — you're not expected to graduate and all of a sudden be this amazing contributor right off the bat.
Anne[6:34] What did you find was helpful to actually get competent at the job?
Justin[6:54] A lot of studying. And this probably comes back to that communication factor as well — one thing you can always do in any field is go in and talk to the patient. Start building out that relationship and rapport. You don't need to know anything about a specialty to go in and start a conversation. A lot of PAs come out very good at taking histories and doing physical exams, and maybe you can't put a full plan together or come up with a full differential. But if you're able to be brave and just have a conversation with patients even when you feel overwhelmed, you're way more likely to learn versus just shadowing. If you're just tailing behind someone, you're taking it in, but it's not the same as having to try to do it yourself, making a decision, being wrong, and then learning from that. Take that home, study, get the feedback, then go into the next patient and do it again.
Anne[8:00] How long have you been practicing as a PA now?
Justin[8:00] I graduated in 2013 and I'm still with Dr. Rabinovich now. It's changed a lot, but I'm still working with him in Orthopaedics. We do a lot of procedural medicine. And the pain care since 2016 as well, so I'm just hitting my tenure in pain management too.
Anne[8:16] How would you say your confidence and competencies are now compared to when you first started?
Justin[8:22] It takes a long time to become an expert in the field, and I'm certainly not an expert in Orthopaedic surgery as a whole. There are things we do here — interventional procedures and injections — where I've certainly become an expert. But Orthopaedics as a whole is enormous. Pediatric Orthopaedics, for instance, we don't see a lot of, so I'm nowhere near an expert there. Every specialty has its niche. I do feel very competent in the job I'm doing now in the niche we're in within Orthopaedics and same within chronic pain. But if I were to switch into a different Orthopaedic role, although some skills are transferrable, there would still be a learning curve.
ArthroBiologix: Co-Founding an Outpatient Orthopaedic Practice
Anne[9:18] What is ArthroBiologix before going into how you co-founded it?
Justin[9:25] ArthroBiologix is an outpatient Orthopaedic practice. We specialize in regenerative medicine and treating patients in that middle ground of non-surgical practice. When we were in the hospital in Branford, we were part of a big surgical practice — Dr. Rabinovich is a foot and ankle surgeon. There are pros and cons to working in hospital settings versus private settings. Change can be slow in hospitals because committees are responsible for budgetary decisions and resource allocation. In 2016, when Dr. Rabinovich chose to leave, we wanted to be able to make some of those decisions on our own — to be more responsible for change and make that change fast. We did not appreciate the need for this niche market of outpatient Orthopaedic medicine at the time. When we left, we were seeing 10 to 20 patients a day and it wasn't even called ArthroBiologix. We were doing semi-surgical work — really non-surgical management conversations, counseling, and starting with some injection therapy. That field evolved just in terms of the need and the subset of patients who are maybe followed by a surgeon, waiting for surgery, but don't want surgery or don't qualify. A lot of surgeons have such busy surgical practices, they don't necessarily have time to meet that middle road. That became our specialty. It was a very slow process, which is why I started working in chronic pain because we didn't have enough patients at first. Now we have 20 providers and eight Physician Assistants and we're seeing around 200 patients a day sometimes. It just goes to show you how much need there is in this field of outpatient Orthopaedics.
Anne[11:32] It sounds like it was more of a partnership in terms of co-founding ArthroBiologix. Can you tell us a little bit about what that relationship looks like and why it may not be as conventional as the typical PA/MD supervisory relationship?
Justin[11:57] We see a lot of follow-ups, and although we see a lot of Orthopaedics, we don't subspecialize, so we're seeing a mix of everything — upper and lower extremity. When we transitioned to this outpatient practice, I'd been with ArthroBiologix for almost three years. I think the best physician/PA relationships are built on trust and working like colleagues or teammates rather than an employer-employee relationship. With medical directives, there's a lot of autonomy for PAs depending on the specialty. In our field, patients are looking for good care and to build relationships with a provider. Patients really want to see the same provider — they're not waiting to see the surgeon. A lot of times they don't even want to see the surgeon. They want to see the same PA that gave them a good treatment on their last visit. So we've slowly evolved into a practice where we can see patients more autonomously while working alongside one another. If I have questions or patients want to see the physician, there's certainly continuity of care and he's always there. But we can work alongside each other rather than me seeing someone and him coming in behind me every single time.
Anne[13:28] Most PAs follow a traditional employment path, and your career has taken a bit of a different road. You've co-founded practices and worked across multiple specialties. Was that intentional or did it evolve?
Justin[13:42] Like most careers, it evolved. There was intentionality in choosing Orthopaedics and wanting to work with Dr. Rabinovich in the region I chose. But it was scary in 2016 when he told me he was leaving the hospital — that was like a one or two month notice — and he told me he might not be able to keep me on as a full-time PA because the practice couldn't sustain it. The market for PAs wasn't extremely hot at the time. It just so happened this opportunity opened up in Burlington at the pain care clinic where an international medical graduate was working and had gotten into a residency. They were looking for someone to fill that position, and the timing blended well between working part-time there and part-time with Dr. Rabinovich at ArthroBiologix. That set sail into some medical legal work, and working in intake assessments for the motor vehicle accident industry at the pain care clinic is where I started doing some Botox management for prophylactic migraine treatments. Just being introduced to new people along the way, I've had the fortune of having so many great mentors. Some that provide Botox cosmetically gave me a nudge to say you should be trying this. I hesitated for so long, but eventually with the help of some of these mentors, I took the leap and started the Hamilton Botox aesthetic medicine venture. Without doors closing and leaving the hospital, I never would've been in pain care. Without being in pain care, I never would've used Botox. There's intentionality in making decisions and choosing to walk through some of these doors, but the doors also have to open up and present themselves.
Finding PA Mentorship through Networking
Anne[16:02] For new grads who want to network — maybe not with the intention of jumping into another field, but wanting to build relationships and find mentors — what advice would you have?
Justin[16:24] Much like yourself, when we graduated there were none of us. There were no Orthopaedic PAs in the field of procedural medicine and really no one to ask questions to — even from a financial perspective when it came to just advocating for yourself and your worth. But now there's a lot of us. Many people here may know of the OrthoPA Network, run by Ohood Elzibak, and it's amazing — a great resource for up-and-coming PAs, current PAs, and practicing PAs to come and explore and meet other PAs working in the same field. It's a great place to find mentors. There are PAs who've been in the field for one or two years, but also 10-plus years now. It's a great way to meet potential mentors and get guidance on salary negotiation and even entrepreneurship. There are a lot of resources when it comes to PAs who have paved the path before you, and being able to communicate with them is invaluable.
Building Competency in Procedural Medicine and Ultrasound-Guided Injections
Anne[17:41] You do a lot of procedures — that seems to be your niche. What drew you toward procedural medicine and how has ultrasound specifically impacted your clinical work?
Justin[17:57] Anybody who's followed OrthoPA Network or my page knows I love ultrasound. I've always loved procedures. I thought I'd go into emergency medicine — it just didn't present itself location-wise when I graduated. But I love the portion of medicine where you have an acute issue and you can do something about it physically with your hands and change it — whether that's suturing a laceration, splinting a fracture, or doing an injection. There's this concrete before and after, an immediate change, immediate benefit and satisfaction in those procedures. I personally love working with my hands, and it fits very well with this aspect of medicine. I love the fast-paced nature — seeing patients and doing something over 10, 15, 20 minutes and then seeing the next patient. You build a little rapport but there's not this long hour-long session, which some people love and are meant to do. For me, I love the acuity of it. When it comes to ultrasound, it has revolutionized the way we practice in Orthopaedics. When I graduated 12, 13 years ago, we were doing a lot of blind injections — no ultrasound at all — for foot, ankle, knees, and shoulders. Once we started using ultrasound and became competent with it, the accuracy of injections went way up, the efficacy went way up, and the comfort for patients during the procedure significantly improved. Now at ArthroBiologix, we have eight or nine ultrasound machines and PAs that train with us only ever use ultrasound. It's actually become something of a joke here that the PAs can't do a blind injection — they don't even know how to landmark properly, which is a good thing. It'll just become common nature to have a procedure done under radiographic guidance rather than blind.
Anne[20:09] The hospital I work at — about 50% of surgeons do it blind, and a smaller percentage use ultrasound guidance, otherwise we're referring out to interventional radiology. For PAs who want to build competencies in performing procedures, what does the process of becoming good at that skill actually look like in real life?
Justin[20:35] At the beginning when you're learning a new skill, it feels very manual. Using ultrasound-guided injections as an example — you're thinking about your landmarks, sterility, the angle of your needle, how to position the patient, what to say to the patient, what could go wrong. There are a lot of steps. My wife Deanna Lautenbach is one of the clinical chairs at McMaster's PA education program and took her master's in education. She introduced me to the concept of "see one, do one, teach one." That's a little old school. It's probably better to think of it as see a few, and then break the skill down into smaller chunks. For an ultrasound-guided injection, you're not going to watch someone do one and then step in — the number of steps is considerable. Break it down: how do I hold the ultrasound? How do I position my hands on the patient to get the image I'm looking for? That step alone is something you can practice on your own. Get a model and practice just the injection. How do I get needle gain under the ultrasound machine? How do I dynamically change the ultrasound during the injection if I lose needle gain? Then how do I do all of this while I sterilize the field, uncap my needle, position it — and then you bring all those steps together. Comfort comes from repetition, but competence comes from good feedback. You want to have someone watch you do a procedure multiple times and give you feedback. Without feedback, you become comfortable but not necessarily expert. The more you can have an expert watch you, the better you'll get.
Anne[22:45] I often compare reading an ultrasound to looking at a snowstorm and trying to understand what's happening. How did you learn ultrasound interpretation in addition to the procedure itself?
Justin[22:57] Totally agree. As Physician Assistants and physicians, we read a lot of x-rays, MRIs, and CT scans, but for some reason we don't read a lot of ultrasounds. 10 years ago when we started using ultrasound, I felt exactly the same — so intimidated. I was comfortable doing it blind and had a bit of pushback against adopting this new skill because I had no idea how to use it or what I was looking at. A lot of this just comes on the job. When we break down ultrasound — and I'm developing an ultrasound course — we're trying to get beginner injectors to have an approach to an injection and have pattern recognition. It's not about being able to perform an ankle and a knee and a shoulder all at once. It's: what does tissue look like? What does fat look like versus tendon versus muscle versus bones and joints? Once you can recognize those patterns and build your anatomy knowledge, you can start transferring that knowledge onto the ultrasound machine. Once you can do that, the injection skill is just the next step. A lot of it is just pattern recognition. It was intimidating at the beginning, but the more times you see it, the more comfortable you feel.
Anne[24:30] So it wasn't necessarily a course or certification — it was more doing and learning as you go?
Justin[24:36] There are courses you can take to get better at ultrasound, but there is no certification in ultrasound — there's a very high-level musculoskeletal ultrasound certificate that something like an ultrasound technician would have, but beyond that there's no stepwise approach. One of the reasons I've started developing a beginner-level ultrasound course is that the courses available are very expensive. I'd love to have something just for beginners to introduce them to ultrasound, get them comfortable with pattern recognition, have some general approaches, and give them hands-on time scanning — because that's what people need. Part of my rationale is wanting to tailor this to whatever practitioners need, whether they're scanning just shoulders or just hips or just knees in their practice.
Anne[25:38] What are the specific learning gaps that you were trying to address when you developed that ultrasound course?
Justin[25:56] What we want to do is have a simplified scanning framework. When you're scanning a joint or grabbing an ultrasound machine, you should have a solid idea of how to position your patient, how to hold the probe, and how to place the probe to get the best view possible. We don't have a lot of time in medicine, and the ultrasound adds another step. Bringing that step in when you're already comfortable without it can slow you down at the beginning. So we want to create repeatable protocols where practitioners feel comfortable grabbing an ultrasound machine and understanding the pattern they're looking for — mental checklists: how is the patient going to be positioned, how am I holding the probe, what's the picture I'm looking for? Some of the common gaps I see are needle trajectory — what degree to use to get the right angle down to whatever structure you're injecting — and what to do when you lose visualization mid-procedure. And then at a next level, how do you manage the patient's anxiety during the procedure? Because it's not always going to go well, and you have a real patient sitting in front of you feeling anxious. When patients feel anxious their tone goes up and oftentimes their pain is worse during the procedure. You've got to manage that at the same time.
Anne[28:10] If someone is interested in taking an ultrasound course with you, how would they go about doing that?
Justin[28:10] OrthoPA Network is going to be starting a more formal course introduction in the fall and maybe in the spring as well — the intention is to run a couple of courses a year. We're also trying to open the door to training and shadowing. I personally have no problem bringing on learners and practicing PAs in the practice who want to come and watch how we do things here at ArthroBiologix. If anyone wants to reach out personally, I'm okay with that. We can leave my email in the show notes.
Orthopaedics vs. Chronic Pain: Differences in Approach
Anne[28:50] You work in both Orthopaedics and chronic pain, which from my experience are very different patient populations with different approaches and different outcomes. How do those mindsets differ?
Justin[29:09] When people think of Orthopaedics, they think of broken bones and surgery — that timeline of three to six months where you have a problem, identify the structural pathology, and do something to correct it — whether physiotherapy, strength training, a procedural thing, or surgery. You're trying to restore function. It's very targeted: what's broken, how do we fix it, how do we restore function. In chronic pain, the pathology is often multifactorial. You're dealing with more than one structure, multiple systems — GI and neuro involvement, multi-joint involvement, potentially autoimmune mediated, and neurologically amplified pain. A lot of times pain is out of proportion to the imaging. You might see someone with very mild degenerative change having severe pain. In chronic pain you're dealing with much longer timelines, fluctuations in pain, sleep disturbances, mood interactions, and patients who are living in fear of pain — fear avoidance. A lot of times we're dealing with medication strategies. Our Orthopaedic patients often start falling into this chronic pain pattern too, especially with older patients with degenerative conditions. You learn how to have in-depth communication, longitudinal thinking, and expectation management. You learn to appreciate the small wins — that there's not always a fix. It's not necessarily going to get back to normal. It's learning to manage and live with some pain. Chronic pain management has really helped me in dealing with our Orthopaedic patients as well — both fields are different but there's crossover, and I think each has helped me in the other.
Anne[31:50] In chronic pain, what are the types of injections that you do?
Justin[32:05] A lot of chronic pain management is neck and back involved — it's harder to treat surgically, so patients end up with these chronic pain pictures, especially if there's nerve involvement. At our pain care clinic, we use radiographic guidance with x-rays, so we don't do facet injections or medial branch blocks. There are some pain clinics that do very high-level interventional procedures. We do perform some paravertebral blocks around the lumbar spine and some joint injections there as well. One of the bigger areas for us in chronic pain is migraine management. Migraine management is treated with a combination of oral medications and behavioral changes, but for people who fail medications, we perform Botox injections — botulinum toxin injections for migraine management under a very strict preempt protocol where we inject very specific values of Botox units into very specific targeted areas. It's an amazing treatment. Patients come every 12 weeks for repeat treatments. That's something I've been working with for the last 10 years.
Anne[33:16] How does Botox work in chronic pain?
Justin[33:27] I could be corrected here — but I do not believe we fully understand the mechanism of how Botox addresses migraine management. Botox has been around for 20-plus years, and it did start in the cosmetic industry. What was found was that patients getting Botox for cosmetics were getting fewer headaches. So they started branching out and treating various muscles around the head and face, and developed this protocol that reduces headaches for 12 weeks. We are still turning off muscles, and it depends on the cause of the migraine, but we don't fully understand how the Botox turns off the migraines. It started with the cosmetic industry and patients getting improvement in their migraines, and then branched out until we developed this protocol we use now.
Anne[34:19] And is it OHIP covered?
Justin[34:21] The Botox itself is not OHIP covered. The procedure is covered by OHIP, so getting the injections done is covered, but the Botox itself is not. So patients either pay through third party coverage or pay out of pocket — they pick it up at a pharmacy and bring it to the office, and then we inject it.
From Botox for Migraines to Aesthetic Medicine
Anne[34:39] So how did treating migraine patients lead you toward aesthetic medicine?
Justin[34:43] The whole field of aesthetics is not something I'd ever really thought of. Cosmetic patients in the past were getting benefits with migraines, and that's how this preempt criteria and the development of Botox for migraine management came about — but in reverse, at our clinic I'm treating patients with migraines and they're getting cosmetic benefits. A lot of them really love those cosmetic benefits. My supervising physician would often do a couple of little touchups outside of the protocol, strictly for cosmetic purposes. I learned to appreciate that cosmetic piece. It's less complicated than people may feel it's made out to be, and I became more comfortable with it because we were treating so many migraine patients. One of our physicians has a wife who's a nurse practitioner and medical director for a number of nurse injectors. I had the opportunity to meet her, and in that simple relationship she said, I think you would be a great injector. I love your personality, you have the skill set, you're already using Botox. She said I should take some formal training and consider doing Botox on the side. It took me a little push because I wasn't sure that's what I wanted to do, but I committed and took a training course through the National Academy of Aesthetic Medicine with Dr. Rosati in Vaughan. I learned the general principles for cosmetic medicine that I didn't have before. And from there it's just been a slow evolution — treating some friends, then family, and now there's a business and things are growing.
Anne[36:36] A friend of mine who's a PA from the States talked about how aesthetic Botox is a lot like artistry. Would you say that's a fair comparison?
Justin[36:47] Absolutely. And it's something I am still very much learning. As much as those guiding principles are there, competent injectors who've been using Botox for a long time are playing outside of those principles all the time because everyone's face is different. It's not as simple as landmark, put in a certain number of units, and move on — not at all. Everyone expresses their face differently, with different muscle strength and different movements, whether that's in their forehead, crow's feet, or frown lines. Some people have asymmetric faces. You really need to assess a patient before you can tell them how many units they're going to get or offer a treatment plan. And I'm not an expert here yet — not even close. But in seeing a lot of different faces, I think it takes a thousand faces before you start feeling comfortable seeing those patterns. And then patients have different expectations and want different things — some want very subtle transitions, some want a more aggressive treatment. So you have to have open, transparent communication about what they want and what you can and can't offer. This field is for sure an art.
Anne[38:28] What are some of those advanced cosmetic injections?
Justin[38:30] Some people are doing fillers and collagen-stimulating products to help treat parts of the lower face and neck. Some people treat their lips — fillers in the lips and cheeks — and again there's very subtle filler and very aggressive filler. Then you get into more surgical procedures like threads and obviously plastic surgery and facelifts. And then there's a lot of the medi spa type work with lasers, microneedling, and peels. There's a whole menu of options. For Hamilton Botox, I'm really looking to treat a subset of patients seeking a natural effect with Botox. I'm not sure I want to get into the next level of this industry. I think a lot of people land in that same place. I'd love to be an expert in that niche and maybe not expand into offering absolutely everything to everybody. But I'm still learning and growing, so I don't know exactly where that niche is going to land.
Founding Hamilton Botox: Running a PA-Led, Physician-Directed Aesthetic Business
Anne[39:30] It sounds like you founded Hamilton Botox. In Ontario, PAs cannot own independent practices, so you had mentioned it's physician-directed. What does that model look like day to day?
Justin[39:47] Just like working in medicine, there are medical directives that I practice under. Taking the training course through the National Academy doesn't give me the right to go inject Botox on my own — I still work as a Physician Assistant and have to work under somebody's medical directives. I'm fortunate that one of my colleagues at ArthroBiologix has a mother who's a family physician and offers cosmetic procedures including Botox in her practice. I reached out and she was willing to be a medical director for me. She came and watched me treat three or four patients, seeing my full approach — counseling patients, communication, signing consents, using an EMR, performing the actual procedure, and seeing some outcomes — and she felt comfortable. We built a relationship where I practice under her medical directives. It's not dissimilar to the medical directives I would use for migraine treatments at Burlington Pain Care. It's just on the cosmetic side. As a Physician Assistant practicing it, it actually looks the same, which is interesting. That took a little bit of research because there's not an abundance of PAs working in a private industry like this, but I'm not the first to do it. It did take some investigating to find out how to go through the proper channels.
How PAs Can Get Started in Aesthetic Medicine
Anne[41:06] If an experienced PA not working in cosmetics was thinking about doing something similar, what would your recommendation be in terms of how to get their foot in the door of aesthetic medicine?
Justin[41:17] If they're working in a practice where someone they work with is already doing cosmetic injections, I think it's a very easy transition because that person's probably willing to be a medical director. That's probably the biggest hurdle — finding a medical director. I struggled early on because at Burlington Pain Care, where we treat migraine patients, they weren't doing cosmetic procedures as a niche — they were doing migraine prophylactic treatments, and then patients might get a little Botox for cosmetics here and there, but they wouldn't call themselves cosmetic injectors working in aesthetic medicine. As a Physician Assistant, you want your supervisor to be in the field you're practicing in. As much as they were qualified to inject Botox, they wouldn't have said they were experts in aesthetic medicine. That's what led me to find my current supervisor who does practice in the field regularly. Should the college ever ask me or want to see my medical director, our practices align and she's an expert who can provide that expert opinion before injections, after if there were complications, or during a procedure. If you don't have a supervisor in that niche or field, reach out to me — or find someone else providing Botox. It's a lot easier having someone who has already crossed some of these hurdles. I've had a couple of PAs reach out via online messenger and email and I'm happy to answer those questions.
Aesthetics: The Business Side of Medicine
Anne[43:05] Hamilton Botox is a very entrepreneurial endeavor. There's a whole business side that you aren't necessarily taught in school. What were some of the big business decisions that you had to learn and figure out on your own?
Justin[43:28] I feel very blessed and fortunate that I've had some amazing mentors, Dr. Rabinovich included as probably one of the biggest, but also some close friends and other supervising physicians. I don't know anything about business. Financial literacy is not something I would claim to be an expert in, but as a PA it's important to be aware of it when negotiating salary and building your role within a system. Starting a business is something completely different beyond that. I felt so naive after I took that training course — I thought I'd take it and then be able to provide Botox to patients. But there are so many steps and I can appreciate why so many people with a dream never pulled the trigger, because it is so intimidating. One of the biggest decisions was actually incorporating — how do you become a business? I have a close friend who's an accountant who helped me go through the steps of incorporating and filing taxes for the first time. Then how do people know who you are? Social media is not my jam at all, but it's part of the role. How do you create a Google business profile? How do you create an Instagram or LinkedIn page? Developing a webpage that people can land on and see your work. How do you set up a phone and get people to reach you? And then how do you actually order supplies? As a Physician Assistant, I found it very hard to reach out to pharmaceutical reps and order Botox, so I had to find a third party connection. Businesses are not profitable up front — these steps have costs associated with them. There's a big personal investment upfront. If I'd been aware of all of those steps from the beginning, I think I would've been more hesitant. But I've just taken them in stride — every time something came up, I said let's sort this out and move on. If you overthink it, you could talk yourself out of it. There are people that have done it before so you're not paving the path for the first time, and there are people willing to help even if you don't personally know them.
Anne[46:43] If someone were interested in starting a business, what would you recommend as first steps?
Justin[46:52] There are companies out there that will help you organize a business from start to finish — creating a business name, incorporating, and filing taxes for the first time. That could be very helpful if you don't know anyone who does these things. Also just reaching out to an accountant — they do so much. There are platforms like Squarespace and GoDaddy that will create websites for you and help you incorporate as well. Having an accountant is just incredibly helpful. I would not try to do it on your own — I don't even know if I could do it again alone. It's very complicated. So asking for help and hiring help is a necessity.
Anne[47:50] It takes a village. And being the best version of yourself is surrounding yourself with people that can help you grow.
Justin[48:00] I like to focus on the things I'm really good at — that's seeing patients, doing Botox, and doing injections. And then there are things I'm not good at — social media, online business development, accounting. There are people that are experts in those fields. Let the experts do their thing and focus more on the things you're passionate about and good at. That's probably the right way to go for most things.
Managing Multiple Clinical Roles without Burning Out
Anne[48:26] You manage multiple clinical identities — parallel clinical roles across very different practice environments. How do you manage that without it becoming unsustainable or burning out?
Justin[48:39] This is a good question and I've flirted with burnout in the past. Even just stepping into a leadership role through ArthroBiologix — when you graduate, I think that should be your main focus. We talked about that six-months-to-two-years period to feel competent and really expert in your field. But there are expectations when you're employed — see a certain number of patients, perform a certain number of procedures. And when you take on a leadership role like training PA students, that expectation doesn't go away. You're just adding the student on top of it. Organization is not my strongest suit but I've learned to become better at time management. You need to be efficient when it comes to paperwork and seeing patients. I enjoy having students and clinical placements come through — it brings me joy even though it's more work, and you learn to balance it. You schedule your work life around those things. I may book fewer Botox things that week or have fewer meetings. I feel very competent in my job at ArthroBiologix and Burlington Pain Care — the technical work I'm doing day-to-day isn't something I have to think hard about anymore. When those things become more second nature, you start to relax a little bit, you have better conversations with patients, and you're able to communicate better with colleagues and students. If you were always stressed in the work you're doing on a day-to-day basis, I think that would lead to burnout. Adding Hamilton Botox on top of everything has been a lot, but it's something I'm very passionate about. You can't have your hands in every single pot because you will burn out regardless of how much value you put to it or how much money you're making. It's something I'm always thinking about and trying to balance. I have an amazing wife who helps balance things as well. It's a constant change — you always have to sit back, reevaluate, and see where things are at.
Anne[52:12] While you were speaking, it made me think — some PAs pursue the profession because of better work-life balance. Would you say there's such a thing as that, being a PA or any healthcare provider for that matter?
Justin[52:26] I am personally seeing more new grad PAs do it better. I think that's a great change. When Anne and I were first graduating, the expectations were very high and there weren't an abundance of places you could go, so you just had to take it in stride. Whereas now there's more opportunity and PAs are able to better leverage that. More opportunities means more leverage. PAs know their worth a bit more. The OrthoPA Network and the PA consensus salary are amazing resources for PAs to have an idea of where they should be starting and how they should be growing. This next generation of PAs values their time more. People are willing to come to work and work hard, but they don't want to work 60 hours a week. Here we have PAs that work three days a week, four days a week, five days a week, and even casual part-time one or two days a week. You can find it. But you've got to balance that with your own personal financial life goals and family. Medicine is not easy and resources are very limited, especially in the next two to three decades. There's not enough providers and there are a lot of patients. But it's challenging and you have to find time outside of work. The day-to-day grind in medicine is always busy for sure.
OrthoPA Network: Building a Community of PAs
Anne[54:36] You've mentioned OrthoPA Network a couple of times. Can you tell us what it is and what your role is within that organization?
Justin[54:44] About three years ago, Ohood tapped me on the shoulder and asked if I would be a member of the OrthoPA Network as a finance lead. Ohood is creating OrthoPA Network as a community hub — developed by PAs, for PAs — to encourage learning and collaboration among Orthopaedic PAs. There's a lot of us now, which is amazing. It's bringing that community together and creating a learning environment suited for PAs in a way that can be provided for free or at very low cost. In order to do that, you have to find resources — things are not done for free. Part of my role is finding sponsors, often pharmaceutical or industry reps, that partner with us, advertise through us, or sponsor events. In return, they may get an opportunity to speak to PAs and develop a pool of people they can show their product to. In doing so, we're able to provide education for free a lot of the time. I love what Ohood is doing — it's an opportunity to build this community of PAs that can collaborate together.
Anne[55:59] CME and continuing professional development credits are a requirement for maintaining your PA license, and they tend to be very expensive, so it's great that they're able to offer it free.
Advice Justin Would Give to His New PA Grad Self
Anne[56:12] If you were to speak to your 2013 new grad self, what would you say?
Justin[56:19] I'd given this some thought recently and I would tell myself it's worth it. Medicine is hard — it's busy and it's a grind — but I wouldn't change my decision. I don't regret becoming a Physician Assistant at all. It's very hard, but it's very rewarding. As one of the early graduating classes, we've seen PAs grow so much and just change the entire field of medicine. When we graduated, a lot of people didn't know what a Physician Assistant was. We spent every day with 80 to 90% of our patients trying to explain what a PA was before we even got into treating them. And now it's rare that I meet someone who hasn't met a PA, been treated by a PA, or at least knows what a PA is. I love that we're part of that groundbreaking new profession. I love the satisfaction I get out of work. I wouldn't go back and change anything. Being a Physician Assistant is awesome.
Anne[57:23] It sounds like you wouldn't have changed anything about your path.
Justin[57:28] It's hard to know, but I like where I'm at. People say you can't shoot for the stars when you graduate — you don't know what's available to you, you have to start somewhere, start in whatever field you feel passionate about. If you're passionate about your work and you love being a PA and you work hard, doors are going to open and opportunities are going to present themselves. There's some risk tolerance involved. But being willing to walk through some of those doors — I wouldn't have dreamed this is where I would be in 2013 when I graduated. If I could look back and see myself in the future, it'd be amazing. I love where I'm at. And to think of where 20 years from now is going to be for the PA profession and PA education in Canada — it's amazing.
Challenges of Pioneering the PA Profession in New Provinces and Territories
Anne[58:34] I was speaking to new PA grads from programs just established in new provinces — Saskatchewan, Dalhousie, Calgary. A lot of them are experiencing what we experienced as part of the first couple of classes. What would you say to them about not getting discouraged, given the journey you've gone through?
Justin[59:07] It's amazing that we have so many schools popping up and graduating PAs. I feel for the educators — starting these programs with so little resources and establishing a program from scratch is so hard. I look at where McMaster's and Toronto's PA education programs are at and they've been around for 15-plus years. That's a lot of work. So to the educators out there, please keep building these tools because these are the tools we need to put PAs out there. For the PAs themselves — stay strong and steady. The profession is amazing and people will see that. It can be defeating when you're explaining your role and people don't appreciate what a PA is. You're responsible for educating the general population. But on the other side of that, you are the leaders of the profession at this time and you will be ahead of everybody else. That presents opportunities too. A lot of times being first leads to opportunities that others may not get — whether in the program and teaching or just being groundbreaking in niche markets like entrepreneurship roles. With challenges come opportunities. Try to seek some of those opportunities.
The Business Case for Hiring a PA
Anne[1:00:49] Orthopaedic surgeons have come up to me and asked about hiring a PA. Some make the comment that PAs are too expensive. Within the context of Ontario, which is fee-for-service for surgical specialties, what would you say to that?
Justin[1:01:12] Hiring a Physician Assistant is an investment and a partnership. I would pressure anyone who said that to just come and look at ArthroBiologix with eight Physician Assistants and see how it's possible. There are financial incentives and even funding for a PA for the first six months now, which covers that window where you don't feel like you're getting the financial return. But once you get through the first six months, having a Physician Assistant can change your practice so much. Whether you want improved quality of life, reduced workload by 20 to 30% — maybe more depending on how good the PA is — you could just take the cost and use that as quality of life. A lot of people are looking for that. At the same time, if financial wash is what you're looking for, PAs are as valuable as the best fellows out there. There's no doubt that in the fee-for-service model, a Physician Assistant can bring in equal or more than their cost on top of reducing the physician's workload. But it needs to be a partnership — you can't hire a PA to simply do all the grunt work because you're going to burn them out and you won't have a PA for very long. PAs now have a much higher level of financial literacy. They understand fee for service, they understand the money they bring in, they understand their leverage. I don't think any physician would ever regret it. I don't think any physician is going to hire a PA and take a financial loss. I would be happy to have this argument with any physician any time, as I have many times, because I hear that argument a lot and it's not founded on anything — just a lack of understanding of how a PA works.
Anne[1:03:49] What kind of mentoring or onboarding can employers do to train PAs up to be force multipliers in their practice and retain them long term?
Justin[1:04:06] In our model now, we have so many staff that PAs rotate around. For a group that's unsure how to use a PA full-time, a shared model between two or three practitioners is a possibility to start. The best way to get value out of a Physician Assistant is to not expect it at the beginning, and to really treat them like a new grad — like a resident — coming through a placement. Going back to our initial conversation, I felt incompetent at the beginning. I was not useful and I wanted to be useful, but you just don't know how. It's like every clerkship placement — by the end of four weeks you feel like you can do some of this, then you get pulled and have to start again somewhere else. Some employers want to recoup that loss right away, and they don't feel like the PA's providing enough immediately. There needs to be an understanding that it's going to take three to six months for a PA to really provide something worthy. For us here, we expect nothing for the first three months. They shadow, they learn, and they start doing a couple of procedures under supervision. They're actually slowing clinic down at that stage. But then you see the transition happen. And once they're trained and have the skills, they don't get stuck doing only the one thing they learned. You get stuck doing the same one thing if no one's showing you anything else and you try to figure it out yourself. There needs to be a period of investment to make them really well-trained in the things you want them to do.
How to Advocate for Your Own Learning
Anne[1:06:17] What can PAs or PA students do to advocate for their own learning?
Justin[1:06:21] Have that conversation right up front. A lot of PAs are getting hired into fields where they've already done placements, which helps. Or they're going into fields where there are already PAs. The hurdles are a lot less in Ontario now. But certainly don't be afraid to advocate for yourself and to know your worth and leverage that. We have this amazing community now — the OrthoPA Network is amazing, and there are PAs working in every aspect of Orthopaedics. You don't have to reinvent the wheel. You can have these conversations and then take that knowledge back and have an open conversation with your supervisor. And if it doesn't feel right, it's probably not right. PAs are a good judge of character. As much as physicians are looking for someone they can share work with, we also have to be willing to share that work. That relationship goes both ways. PAs need to like who they're working with, because that's a recipe for burnout too — if you don't like going to work because you don't like who you work with every day, you can love your work but it makes it hard. We work so closely with those physicians that you want to have someone you get along with. Not every personality meshes with everybody's. You feel that out in the interview. One thing we do here that I think could help a lot of people is a one or two day shadow placement before anyone commits to anything. If they want to just come and spend a day with us, they can. It allows us to feel them out and them to feel us out. It's almost a better interview. Both parties can say: this was great, let's try this for three months as a probation period. It works very well for us. I think if staff were open to a day of just saying come and see what we do here, you gain a lot more than a basic interview.
Final Notes
Anne[1:08:23] We've definitely gone over time, but this was great. Thank you so much for your time, Justin. I really appreciate all the knowledge you had to share. So where can listeners find you or learn more about the work you're doing?
Justin[1:08:50] ArthroBiologix has its own website at orthobiologics.ca, and you can see our whole team and what we're doing there in terms of private outpatient medicine. For anybody listening, I would absolutely love the follow on Hamilton Botox on Instagram — even if you're not interested in Botox, but just curious about how Botox is done or what PAs out there are doing. That's @HamiltonBotox on Instagram. I do have a website as well, hamiltonbotox.ca, but the Instagram handle would certainly be the best way to find me and see some of the stuff I'm putting out there in terms of videos and footage.
Anne[1:09:22] People can find that information in the show notes. We'll also include Justin's info there. Thanks so much.
Justin[1:09:29] Thanks Anne.